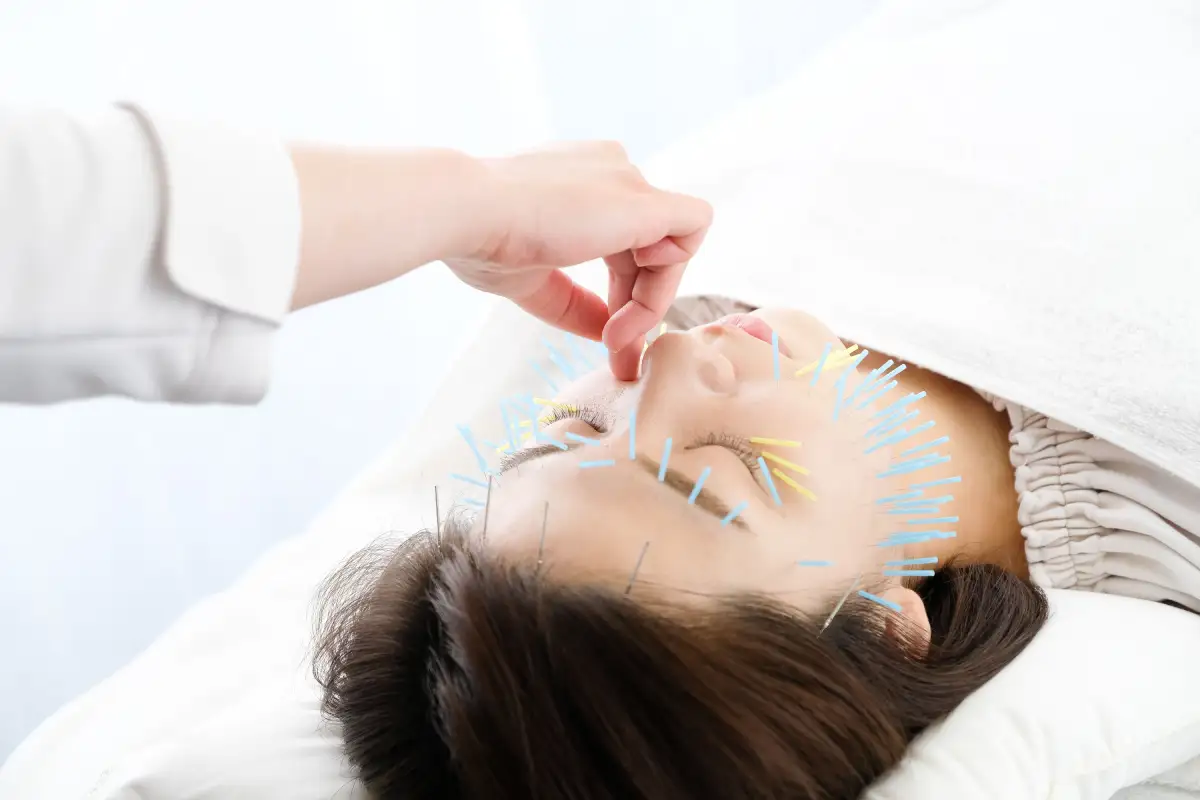
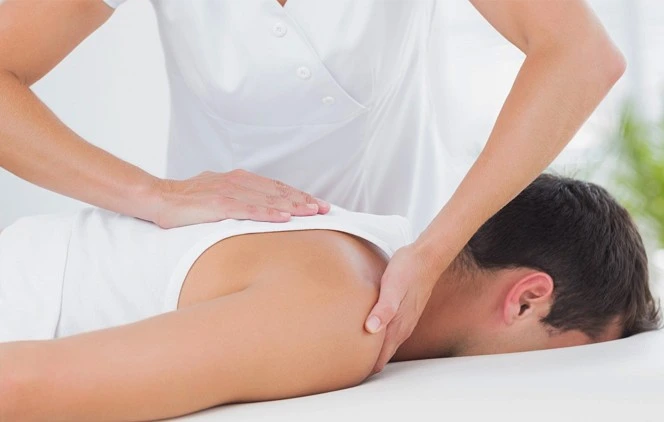
Walking into a clinic with back pain or a stiff shoulder often brings up one big question: should I get an X-ray first? It’s a fair concern. You want answers, and images seem like the logical starting point. But here’s something that might surprise you—most people heading to physiotherapy don’t actually need X-rays beforehand.
Let me walk you through when imaging matters, when it doesn’t, and how physiotherapists figure out what’s really going on with your body.
The Short Answer: Usually, No
Let’s cut straight to it. For the majority of musculoskeletal complaints—think sore backs, achy knees, tight necks—X-rays aren’t a prerequisite for starting physiotherapy. Your physiotherapist possesses the clinical training to assess your condition through hands-on examination and movement analysis.
This doesn’t mean imaging never plays a role. It absolutely does in certain scenarios. But the assumption that you need pictures of your bones before anyone can help? That’s outdated thinking.
What Happens Without Prior Imaging
When you arrive at a physiotherapy Scarborough clinic without X-rays, your therapist conducts what’s called a comprehensive physical assessment. This involves:
- Watching how you move, sit, and stand
- Testing your range of motion in affected joints
- Checking muscle strength and flexibility
- Performing specific clinical tests that reveal underlying issues
- Asking detailed questions about your symptoms, history, and daily activities
This process often tells us more than static images ever could. A picture shows structure. A physical exam shows function.

When Your Body Tells the Real Story
Here’s what many people don’t realize: pain doesn’t always match what shows up on scans. Research consistently demonstrates that plenty of folks walking around pain-free have “abnormalities” on their X-rays or MRIs. Conversely, someone in significant discomfort might have imaging that looks perfectly normal.
A 2015 study published in the American Journal of Neuroradiology found disc bulges in 30% of 20-year-olds who had zero back pain. By age 80, that number climbed to 84%. These findings reshaped how clinicians think about imaging and its relationship to symptoms.
The Hands-On Assessment Advantage
Your physiotherapist’s hands are diagnostic tools. Through palpation—carefully feeling muscles, joints, and soft tissues—experienced practitioners detect tension patterns, inflammation, and movement restrictions that no X-ray captures.
At a quality Scarborough physiotherapy clinic, the initial assessment typically runs 45 minutes to an hour. That’s enough time to build a detailed picture of what’s happening and why.
Situations Where X-Rays Actually Matter
Now, let’s talk about when imaging becomes genuinely important. Certain red flags prompt physiotherapists to recommend or require imaging before proceeding with treatment.
Trauma and Suspected Fractures
Fell off a ladder? Got tackled during weekend soccer? Took a tumble on icy sidewalks (a Scarborough winter classic)? If there’s a mechanism of injury suggesting possible bone damage, imaging comes first.
Signs that warrant X-rays include:
- Inability to bear weight on a limb
- Visible deformity
- Severe localized tenderness over bone
- Significant swelling immediately following injury
- Symptoms following high-impact accidents
Post-Surgical Evaluation
If you’ve had joint replacement, spinal fusion, or fracture repair, your surgeon likely wants follow-up imaging. Physiotherapists working with post-operative patients coordinate with surgical teams to ensure bones are healing properly before progressing exercises.
Suspected Pathology Beyond Musculoskeletal Issues
Sometimes symptoms hint at something more serious than muscle strain or joint stiffness. Warning signs that prompt imaging referrals include:
- Unexplained weight loss alongside pain
- Night pain that wakes you from sleep
- Fever accompanying musculoskeletal symptoms
- History of cancer
- Symptoms that worsen despite rest
- Pain in individuals under 20 or over 55 with new-onset back complaints
Registered physiotherapists Scarborough are trained to recognize these red flags and will guide you toward appropriate medical investigation when needed.
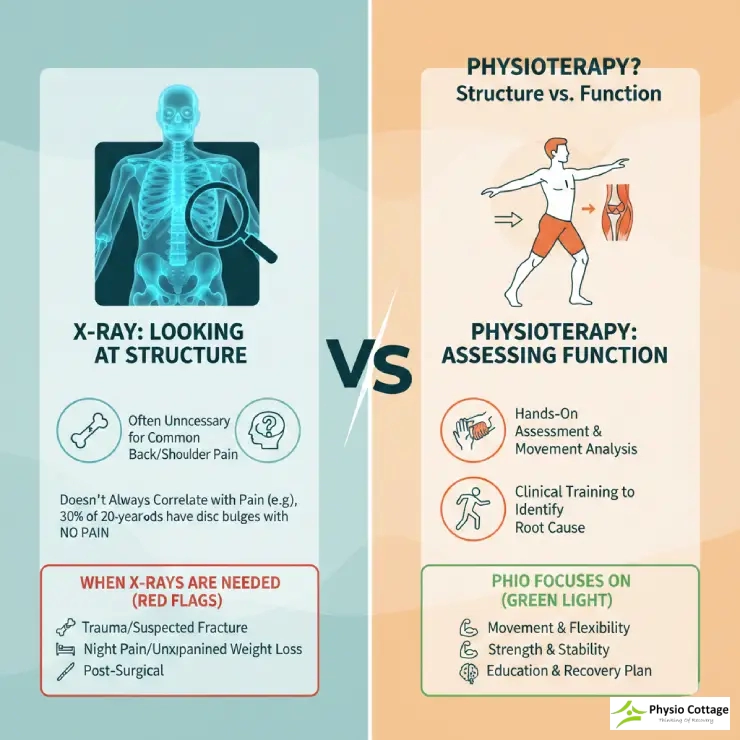
The Problem with Unnecessary Imaging
Getting X-rays “just to be safe” sounds harmless enough. But there are legitimate reasons why healthcare systems globally are moving away from routine imaging for common complaints.
Radiation Exposure Adds Up
Every X-ray delivers a small dose of ionizing radiation. One image isn’t concerning. But people with chronic conditions sometimes accumulate dozens of scans over years. Minimizing unnecessary exposure makes good sense, particularly for younger patients.
Incidental Findings Create Anxiety
Remember those disc bulges in pain-free people? When imaging reveals “abnormalities” that aren’t actually causing problems, patients often become anxious. They start moving differently, avoiding activities, catastrophizing about their spine or joints. This psychological impact can actually worsen outcomes.
Cost and Time Considerations
In Ontario’s healthcare system, getting imaging involves GP visits, wait times, and follow-up appointments. If X-rays won’t change your treatment plan—and for many musculoskeletal issues, they won’t—that’s time and resources better spent elsewhere.
Also Read: What to Expect at Your First Physiotherapy Appointment
How Physiotherapists Make the Call
The decision about imaging isn’t arbitrary. Clinicians follow established clinical reasoning frameworks and evidence-based guidelines to determine who benefits from imaging and who doesn’t.
Clinical Practice Guidelines
Organizations like the Canadian Physiotherapy Association and Ontario’s health quality standards provide guidance on imaging appropriateness. These guidelines synthesize decades of research into practical recommendations.
For low back pain—one of the most common reasons people seek physiotherapy—guidelines explicitly state that imaging shouldn’t be routine for uncomplicated cases in the first six weeks.
The Triage Process
During your first visit, your physiotherapist essentially triages your condition. They’re asking themselves:
- Could this be something serious requiring immediate medical attention?
- Is there a specific structural issue that imaging would clarify?
- Will my examination findings be sufficient to guide treatment?
- Are there red flags suggesting pathology beyond typical musculoskeletal problems?
For most patients walking through the door with garden-variety aches and pains, the answer points toward proceeding with assessment-based treatment.
What to Expect at Your First Appointment
Never been to physiotherapy before? Showing up without X-rays might feel strange, like you’re arriving unprepared. Let me assure you—you’re not.
The Conversation Comes First
Your appointment starts with talking. Your physiotherapist wants to hear your story: when symptoms started, what makes them better or worse, how they affect your daily life, what you’ve already tried. This subjective history provides crucial context for everything that follows.
Movement Assessment
Then comes the objective examination. You’ll likely be asked to move in various ways—bending, reaching, squatting, walking. Your therapist observes quality of movement, notes where you hesitate or compensate, and identifies patterns that reveal underlying dysfunction.
Specific Tests
Depending on your presentation, additional tests might include:
- Joint mobility assessments
- Muscle strength testing
- Neurological screening (reflexes, sensation, coordination)
- Special clinical tests for specific conditions
- Posture and alignment analysis
Diagnosis and Plan
By the appointment’s end, you’ll typically have a working diagnosis and treatment plan. This might involve manual therapy, exercise prescription, education about your condition, and strategies for managing symptoms at home.
For those dealing with ongoing issues, chronic pain treatment Scarborough services often incorporate multiple therapeutic approaches tailored to individual needs.
When Your Physiotherapist Might Order Imaging
Here’s something not everyone realizes: physiotherapists in Ontario can refer directly for diagnostic imaging in many circumstances. If during your assessment something emerges suggesting imaging would be valuable, your therapist can arrange it.
Changing Clinical Picture
Sometimes treatment progresses as expected initially, then stalls. Or new symptoms appear. When the clinical picture shifts in unexpected ways, imaging might become appropriate even if it wasn’t initially.
Confirming Surgical Candidacy
If your condition appears to require surgical intervention—a significant rotator cuff tear, for instance, or advanced hip arthritis—imaging confirms the diagnosis and helps surgical teams plan their approach.
Ruling Out Serious Pathology
Though rare, occasionally assessment findings raise concerns about conditions requiring medical investigation. Your physiotherapist serves as a gatekeeper, recognizing when imaging or physician referral becomes necessary.
Also Read: Struggling to Tell if It’s Back or Hip Pain? Here’s How to Know?
Different Imaging Options Explained
X-rays aren’t the only game in town. Various imaging modalities serve different purposes, and understanding the options helps you participate in decisions about your care.
X-Rays (Radiographs)
Best for: Bone structure, fractures, arthritis, spinal alignment
Limitations: Don’t show soft tissues well (muscles, tendons, ligaments, discs)
Ultrasound
Best for: Tendons, muscles, superficial soft tissues, real-time assessment during movement
Limitations: Operator-dependent, can’t see deep structures or bone detail
MRI (Magnetic Resonance Imaging)
Best for: Soft tissue detail including discs, ligaments, cartilage, muscles
Limitations: Expensive, longer wait times, not suitable for patients with certain implants
CT Scan
Best for: Complex bone structures, detailed fracture assessment, some soft tissue visualization
Limitations: Higher radiation than X-rays, less soft tissue detail than MRI
Your physiotherapist considers which modality—if any—would provide clinically useful information for your specific situation.
Taking a Whole-Person Approach
Modern physiotherapy has evolved beyond simply treating injury sites. The best outcomes come from addressing the whole person, considering how various factors interact to produce symptoms.
A holistic physiotherapy Scarborough approach might examine:
- How your work setup affects your posture and pain
- Sleep quality and its impact on tissue healing
- Stress levels and their relationship to muscle tension
- Movement habits throughout your day
- Previous injuries that might influence current symptoms
This comprehensive perspective often reveals treatment opportunities that imaging never would.
Real Experiences: What Patients Say
Maria came in convinced her knee needed an MRI. She’d been limping for three weeks after twisting it in the garden. Assessment revealed a minor medial collateral ligament strain—something that responds beautifully to physiotherapy without any imaging.
“I was ready to push for a scan,” she admitted. “But within four sessions, my pain had dropped by half. Six weeks later, I was back to hiking. Turns out I didn’t need pictures—I needed treatment.”
David’s situation differed. His chronic low back pain had several characteristics prompting his physiotherapist to recommend imaging: night pain, unintentional weight loss, and a previous cancer diagnosis. X-rays led to further investigation that identified a spinal lesion requiring medical management. Here, imaging proved essential.
These contrasting examples illustrate why blanket policies—always get imaging, or never get imaging—miss the point. Clinical reasoning guides appropriate decisions.
Addressing Common Concerns
Patients often arrive with specific worries about proceeding without X-rays. Let’s address the most frequent ones.
“What if something gets missed?”
Physiotherapists undergo extensive training in differential diagnosis—distinguishing between conditions that look similar. They’re also trained to recognize when something falls outside their scope and requires medical referral. The system has safeguards built in.
“My pain is severe—doesn’t that mean I need a scan?”
Pain intensity doesn’t correlate reliably with structural damage. Some minor injuries hurt tremendously. Some significant problems cause surprisingly little discomfort. Severity alone doesn’t indicate imaging necessity.
“I had imaging years ago—can we use that?”
Old images have limited value for current complaints. Bodies change. New issues arise. If imaging becomes appropriate, recent pictures provide more useful information than ones from your files.
“My friend had the same thing and needed surgery—shouldn’t I get checked?”
Every person’s situation differs. What required surgical intervention for one individual might resolve conservatively for another. Your physiotherapist assesses your specific presentation, not statistical averages.
Making Your Decision
Ultimately, you’re a partner in your healthcare. If you feel strongly about obtaining imaging before starting physiotherapy, discuss it openly with your provider. Understanding your reasoning helps them address concerns appropriately.
That said, consider giving assessment-first approaches a fair chance. Many people surprised themselves—expecting to need extensive investigation, only to find that skilled hands-on evaluation and targeted treatment resolved their problems efficiently.
Your Next Step
Still uncertain whether your condition requires imaging? The straightforward solution involves booking an assessment with qualified professionals who can examine you properly and advise accordingly.
At Physio Cottage in Scarborough, our team welcomes patients at any stage—whether you’re coming straight from injury, arriving with imaging in hand, or simply dealing with nagging discomfort you’ve finally decided to address.
We’ll conduct thorough evaluation, answer your questions honestly, and recommend imaging only when clinical reasoning supports it. Most importantly, we’ll get you started on the path toward feeling better.
FAQ
Can I start physiotherapy the same day as my injury?
For most non-emergency injuries, yes. Early intervention often produces better outcomes. Your physiotherapist will assess whether immediate treatment is appropriate or if you should seek medical evaluation first.
Will my insurance cover physiotherapy without a doctor’s referral?
Most extended health benefit plans in Ontario cover physiotherapy without requiring physician referral. However, check your specific policy details, as coverage varies between insurers.
How many sessions will I need if we skip imaging?
Session numbers depend on your condition, not whether imaging occurred. Simple strains might resolve in 3-5 visits. Complex or chronic issues typically require longer treatment courses.
What if physiotherapy isn’t working—do I need X-rays then?
If you’re not progressing as expected, your physiotherapist reassesses the situation. This might involve imaging referral, but could also mean adjusting treatment approach, investigating other contributing factors, or considering specialist consultation.
Should I bring any medical records to my first appointment?
Bring whatever you have—previous imaging reports, surgical notes, medication lists. This information helps your physiotherapist understand your complete health picture, even if we ultimately base treatment on current assessment findings.
Take the First Step Today
Questions about whether you need imaging shouldn’t delay getting help for your pain or injury. Our Scarborough clinic offers comprehensive assessments that determine exactly what’s going on and what you need.
Book your appointment at Physio Cottage and let our experienced team guide you through the process—whether that means starting treatment immediately or recommending appropriate investigation first.